What is glaucoma?
Glaucoma is a disease of the optic nerve. The optic nerve transmits the images you see from the eye to the brain and is made up of many nerve fibres (like an electric cable with its numerous wires).
Glaucoma damages nerve fibres, which can cause blind spots and vision loss.
Glaucoma is usually related to the pressure inside the eye, known as the intraocular pressure (IOP). When the aqueous humour (a clear liquid that normally flows in and out of the eye) cannot drain properly, pressure builds up in the eye. The resulting increase in IOP can damage the optic nerve and lead to vision loss.
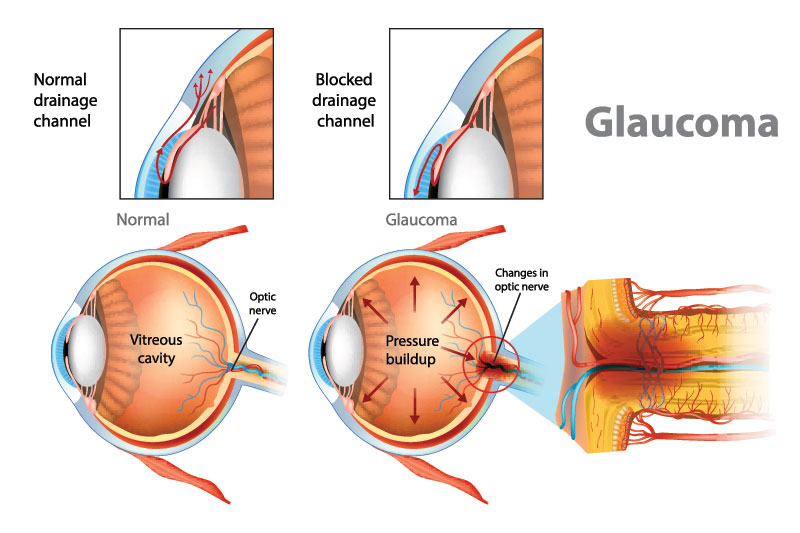
Causes
Open-angle glaucoma
The most common form of glaucoma is primary open-angle glaucoma. In this type of glaucoma, the aqueous fluid (thin, watery liquid in your eye) is blocked from flowing out of the eye at a normal rate through the tiny drainage system.
Most people who develop primary open-angle glaucoma notice no symptoms until their vision is impaired.
Ocular hypertension (or high internal eye pressure) is often a precursor to actual open-angle glaucoma. When ocular pressure is above normal, the risk of developing glaucoma increases.
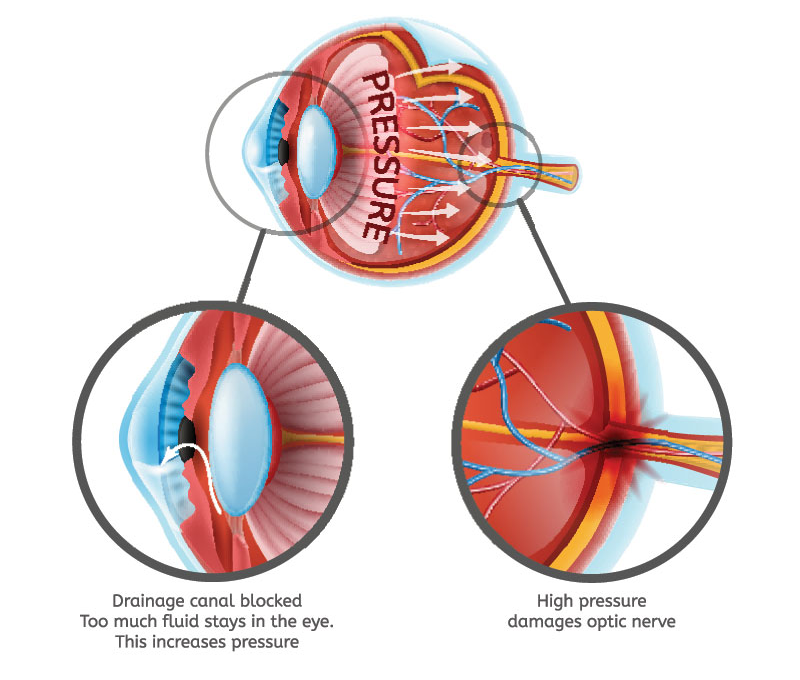
Angle-closure glaucoma
In angle-closure glaucoma, the iris (the coloured part of the eye) may completely close off the drainage pathway, abruptly blocking the flow of aqueous fluid and leading to a sudden increase in intraocular pressure (IOP). This condition is considered an emergency because optic nerve damage and vision loss can occur within hours of the problem.
Symptoms can include nausea, vomiting, seeing halos around lights and eye pain.
Normal-tension glaucoma
Even some people with “normal” IOP can experience vision loss from glaucoma. This condition is called normal-tension glaucoma.
In this type of glaucoma, the optic nerve is damaged even though the IOP is considered normal. Normal-tension glaucoma is not well understood, but lowering IOP has been shown to slow progression of this form of glaucoma.
Childhood glaucoma
Childhood glaucoma, which starts in infancy, childhood or adolescence, is rare. Like primary open-angle glaucoma, there are few, if any, symptoms in
the early stage. Blindness can result if it is left untreated. Like most types of glaucoma, childhood glaucoma may run in families.
Risk Factors
For people with elevated intraocular pressure (IOP), some of the risk factors that will affect whether you will develop glaucoma include:
- Your level of IOP
- Family history of glaucoma
- Your corneal thickness
- Certain optic nerve conditions
- If you are of a particular ethnic background (African American, East Asian)
- Advanced age
If your risk is high, treatment to lower your IOP to prevent future damage is recommended.
Diagnosis
Since glaucoma has no noticeable symptoms, it is a difficult disease to detect without regular, complete eye exams. Ongoing monitoring is needed to watch for changes. During a glaucoma evaluation, you may have the following tests:
- Tonometry to test eye pressure
- Gonioscopy to determine eye drainage angles
- Ophthalmoscopy to assess optic nerve appearance
- Visual field test to assess peripheral vision
- Optical coherence tomography to assess the thickness of the retina
and optic nerve
Tonometry
Tonometry measures your eye pressure by determining how your cornea responds when an instrument (or sometimes a puff of air) presses on the
suface of your eye. Eye drops are usually used to numb the surface of your eye for this test.
Gonioscopy
Your eye’s drainage angle is the area where fluid drains out of your eye. During gonioscopy, you sit in a chair facing the microscope used to look inside your eye. You will place your chin on a chin rest and your forehead against a support bar while looking straight ahead.
The goniolens is placed lightly on the front of your eye, and a narrow beam of light is directed into your eye while your doctor looks through the slit lamp at the drainage angle.
Drops will be used to numb the eye before the test.
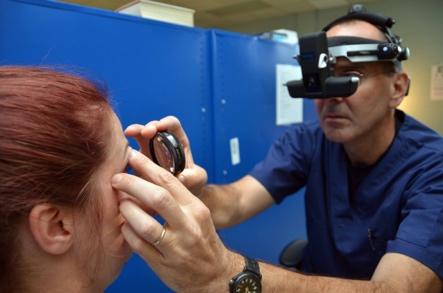
Ophthalmoscopy
With ophthalmoscopy, a high-powered lens is used to examine the optic nerve and retina.
Sometimes computerized images of the optic nerve are taken to inspect the nerve more closely for damage from elevated pressure in the eye.
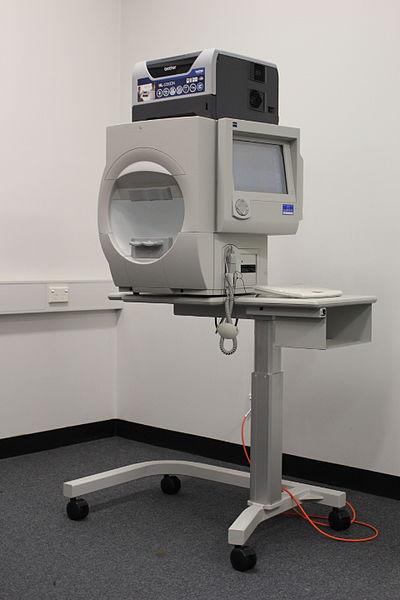
Visual field test
A visual field test can help fi nd certain patterns of vision loss and is a key way to check for glaucoma.
It is very useful in finding early changes in vision caused by nerve damage from glaucoma. This test is done seated at a bowl-shaped instrument called a perimeter. While you stare at the centre of the bowl, lights flash. Each time you see a flash, you press a button. A computer records the location of each fl ash and whether you pressed the button when the light flashed in that location.
At the end of the test, a printout shows if there are areas of your fi eld of vision where you did not see the flashes of light. This test shows if you have any areas of vision loss. Loss of peripheral vision is often an early sign of glaucoma.
Optical coherence tomography (OCT)
A healthy retina (the inner layer of tissue that lines the back of the eye) is only ¼ of a millimetre thick, but it contains multiple layers of specialized cells.
One layer converts light into nerve signals, another processes the nerve impulses, while another transmits these processed impulses to the brain where they are interpreted.
Some tests may need to be repeated on a regular basis to monitor any changes in your vision caused by glaucoma.
Treatment
Glaucoma is a chronic disease. While there is no cure for glaucoma, it can often be controlled with proper management.
The goal of glaucoma treatment is to lower your eye pressure to a “target pressure”. This is a level of pressure that is less likely to cause further optic nerve damage. The target pressure differs from individual to individual. Your target pressure may change during your course of treatment.
Medications
You may be prescribed a medication to lower your eye pressure when the risk of vision loss is high enough to justify intervention.
Treatment often consists of eye drops, and there are several different medications available for the treatment of glaucoma.
These medications may work by:
1) Decreasing the production of fluid that the eye produces continuously (also known as aqueous humour). The classes of drugs that do this are:
- Beta-blockers
- Alpha-agonists
- Carbonic anhydrase inhibitors
2) Increasing the outflow of the fluid that the eye produces continuously (or aqueous humour). These drugs include prostaglandin analogues.
There may also be combinations of drugs that work together to reduce the production and increase the outflow of aqueous humour.
Laser treatments
Laser treatments may also be used to enhance the drainage of fluid from the eye. They include:
1) Selective laser trabeculoplasty (SLT): A laser procedure to create microscopic bursts of energy in the drainage pathways (the trabecular meshwork) in your eye. These bursts open the drainage holes in the meshwork and allow fluid to drain better through them. This can lower the pressure in your eye and help prevent damage to the optic nerve and loss of vision.
2) Laser peripheral iridotomy: A laser is used to create an opening in the iris (the coloured part of the eye) so that fluid can enter the angle of the eye more easily. It is performed for patients with narrow angles, or angles that look like they might be prone to closure. A special contact lens is put on your eye to help direct the laser’s high-energy beam of light at the iris. The laser makes one or two holes in the iris.
Surgery
For eyes in which drops and laser fail to stop the progression of glaucoma, surgery may be recommended to create a new passage for aqueous fluid to leave the eye. These surgical procedures include:
- Trabeculectomy: A procedure where a flap is created in the wall of the eye to allow controlled leakage of fluid into the tissues (conjunctiva) that surround the eye.
- Seton: Implanting a drainage reservoir behind the eye and connecting it to the angle drainage structures with a tube that is buried in the eye wall. Fluid then drains to the reservoir, where it is absorbed.
- Minimally invasive glaucoma surgery (MIG): This procedure involves inserting tiny devices into the drainage apparatus in the angle to bypass the obstruction and allow the aqueous fluid to drain more readily. There are several devices on the market now, and more are likely to be released in the near future.