What is diabetic retinopathy?
If you have diabetes mellitus, your body does not use and store glucose properly.
Over time, diabetes can damage blood vessels in the retina (the inner layer of tissue that lines the back of the eye). The retina is composed of a network of nerves that sense light and help to send images to the brain.
The damage to retinal blood vessels is referred to as diabetic retinopathy.
The various stages or types of diabetic retinopathy include:
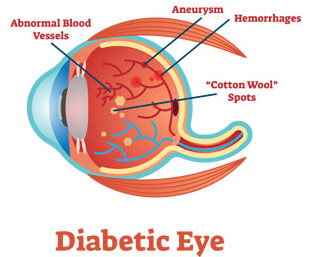
Nonproliferative diabetic retinopathy (NPDR)
In this early stage, tiny blood vessels within the retina leak blood or fluid causing the retina to swell or to form deposits called exudates. Many people with diabetes have mild NPDR that does not affect their vision.
Macular edema
Refers to the swelling or thickening of the macula (the centre of the retina that allows us to see find details clearly) caused by fluid leaking from the retinal blood vessels. This is the most common cause of visual loss in diabetes. Vision loss may be mild to severe, but in the worse cases side vision can continue to function.
Macular ischemia
Refers to the closing of capillaries (or small blood vessels) in the retina. Vision blurs because the macula no longer receives sufficient blood supply to work properly.
Proliferative diabetic retinopathy
Refers to the growth of abnormal blood vessels from the surface of the retina inwards into the vitreous cavity. These vessels are fragile and can break and bleed, obstructing vision or they can produce scar tissue that distorts the retina or in extreme cases causes it to detach from the wall of the eye. These vessels develop as a result of closure of the normal blood vessels in the periphery of the retina as a result of diabetic damage.
Causes
Diabetic retinopathy can arise when you have diabetes mellitus.
If you have diabetes mellitus, your body does not use and store glucose properly.
Over time, diabetes can damage blood vessels in the retina (the inner layer of tissue that lines the back of the eye). The retina is composed of a network of nerves that senses light and helps to send images to the brain.
Risk Factors
If you have diabetes, early detection of diabetic retinopathy is the best protection against loss of vision.
You can significantly lower your risk of vision loss by maintaining strict control of your blood glucose and visiting your ophthalmologist regularly.
People with diabetes should schedule examinations at least once a year.
Pregnant women with diabetes should schedule an appointment in their first trimester, because retinopathy can progress quickly during pregnancy.
Diagnosis
People with diabetic retinopathy may have few symptoms until it is very advanced and difficult to treat.
To prevent progression of diabetic retinopathy, people with diabetes should control their levels of blood sugar, blood pressure and cholesterol. There is considerable evidence to suggest that rigorous control of blood sugar decreases the chance of developing serious proliferative diabetic retinopathy.
A medical eye examination is the only way to discover any changes inside your eye.
If the eye examination finds diabetic retinopathy, you may require a special test called fluorescein angiography or optical coherence tomography (OCT) to find out if you need treatment.
More frequent medical eye examinations may be necessary after a diagnosis of diabetic retinopathy.
Treatment
During the first stages of diabetic retinopathy, no treatment is needed, unless you have macular edema.
Once you have advanced stages of diabetic retinopathy, there may be certain treatments to improve your vision.
Macular edema
Anti-vascular endothelial growth factor (anti-VEGF) drugs
These drugs are the first line of treatment for diabetic macular edema and are injected into the eye regularly to reduce leakage and improve vision (see also AMD for more information on how these work).
Focal laser treatment
This procedure is less commonly used now that anti-VEGF drugs are available.
Macular ischemia
Unfortunately, there are currently no effective treatment options available.
Proliferative diabetic retinopathy
Pan-retinal photocoagulation
This laser surgery may be used to shrink the new, fragile, abnormal blood vessels and reduce the risk of bleeding. During two or more treatment sessions, your doctor places laser burns in the areas of the retina away from the macula, causing the abnormal blood vessels to shrink. While there may be some loss of side vision and night vision, this procedure can prevent severe vision loss.
Vitrectomy
If the bleeding in your eye is severe and does not clear within a reasonable time, or if a retinal detachment is detected, an operation called a vitrectomy can be performed. During a vitrectomy, a retinal specialist removes the hemorrhage and any scar tissue that has developed, and performs laser treatment to prevent new abnormal vessel growth.